Structural problem: our private hands manage our health
- Workers report overflow precariousness, while more and more waiting lists are formed among patients. One of the problems may be the lack of doctors, but when you start looking at the origin of the wound and understanding some clues, you can clearly notice: it's something that has come from a long time ago. The plaster serves nothing. (We have also seen the most significant conflicts of the three capitals: read here).

We are still often told that all this has been caused by the pandemic, which has completely strained the public health system. We are told that waiting lists, in-person consultations, appointments with specialists and the service, public and dignified, will return to that European vanguard that it was before. Three years have passed since we entered home, closed the doors of consultations, delayed operations and entered a situation that seemed to be the end of the world, and continued to affect the consequences. Without going into whether there are three years many or few, it is clear that this justification must one day lose its value, because it cannot always be blamed for the pandemic. Especially if the problem is structural and we do not want to see it.
With the health of the citizens, money can and is made easily, because legislation also allows it. First, the Spanish Constitution does not consider the health of State citizens as a fundamental right, but in the section on social policies it is stated that “all the necessary benefits” will be established for the ordination, management and surveillance of public health. Health is a right, but not a fundamental right. Even if it seems like a fuzzy line, the position and terminology of the article is important when making policies, as history has shown.
From the spectrum of left-wing ideology, it has been denounced for many years, and in the last decade it has again been reaffirmed that the law of new management models of the Public Health System (Decree 15/1997), approved by the Government of José María Aznar in 1997, opened the way for the integration of private companies in health. Or, rather, that decree launched the process of progressive abandonment of the health of citizens in private hands. A few years earlier they had the report of several experts, led by Fernando April-Martorell, who bears the same name: they concluded that the public health system was not profitable and that at that time it did not have a business vision. They suggested the need for external funding and public opinion was disrupted, but the desired response came to it.
A government law of 1997 expressly authorizes the introduction of private hands into the health system
Decree 15/1997 has barely three pages and only one two-point article. The first recognizes more powers for the Autonomous Communities in the field of health, and the second says, verbatim, that the provision and management of health and socio-health services will be provided, in addition to the State's own means, through agreements, agreements or contracts with natural persons, public or private institutions.
The PNV supported the decree along with the two main political parties, and that same year it took advantage of the situation to turn Osakidetza into a private public entity. Since then, Osakidetza has often outsourced the cleaning of health facilities, laundry, the organization’s computer system, as well as ambulances or home services, among others. The public health service wound is not new, although protests by the heads of service at the Donostia Hospital have begun to dance operating theatres to various media.
Unbalanced packaging At the end of the current stabilisation processes, Osakidetza
will have approximately 31,000 stable workers according to the Department of Health of the Basque Government. It will be the highest figure in history, as it has had to stabilise at least three thousand jobs in order to comply with the European guidelines. But it remains to be seen whether it will bring the temporary employment rate down to 8%, as, according to the unions, today it is over 40%.
Besides promoting job precariousness, unstable jobs destabilize the service, as it is not the same as a center having a certain number of workers throughout the year, that in certain times of the year work contracts are interrupted and that the time of the center is reduced. During the past Christmas holidays, for example, in one of every three outpatient clinics, adaptations were made during times, some of which were closed because they were “small”. In summer, one in two health centres suffered cuts – in the words of the Department of Health, “adaptations” – and staff in stable employment were transferred to other centres where it was needed. Of course, those who did not have a stable post, Osakidetza suspended the contract, thus saving a paid holiday.
Between 2016 and
2022 visits to the medical specialist in Osakidetza have been sextized
It is not a new policy: these interventions were carried out before Covid-19. Forcing citizens to move is a sure measure that the service will be more profitable, and that society will have to get used to these “cultural adaptations”, as Health Advisor Gotzone Sagardui implied, “we have to move more”.
Data and figures dance
In addition to moments of emergency, there have been and exist “villages of exception”: in Mendexa and in Amoroto, after two years of protests, they have recently become doctors in the village. They have had to move, but in addition to moving, there are indicators that are often considered as reference data: waiting lists. The interpretations of the figures can be very diverse: one is to compare with those next door and presume to be better, another is to observe the trend of recent years.
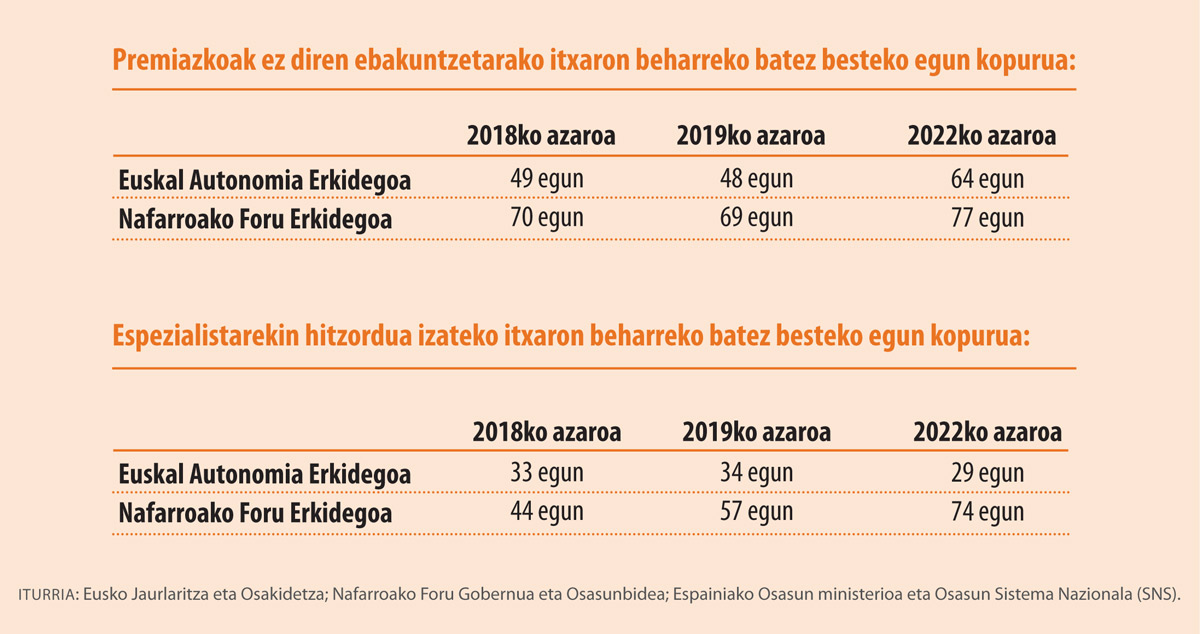
In addition, it would not be better to add a couple of data to the table: since 2016 it has been clarifying that visits to medical specialists in the Basque Autonomous Community have multiplied by six, from just over 15,000 to about 91,000. According to the experts consulted by ARGIA, this increase may be due, on the one hand, to the aging of society and the increased needs and, on the other, to the inability to cope with Primary Care.
On the other hand, there are thousands of citizens waiting for intervention beyond the time that is regulated by law. In the case of cardiac surgery, one in three has spent 90 days and in oncology interventions, 12% have had to wait more than a month.
An example of this is the evolution of the Basque Government Sociometer in the results. Between 2016 and 2021, asking the population of the three territories about the main concerns, between 10% and 11% stated that health was one of them. A year later, according to the latest report published (October 2022), the figure has doubled.
And this concern is reflected in the assessment given to Osakidetza: in 2016 almost nine out of ten claimed that it worked “very well” or “well”, while in 2022 there are seven out of ten who think it and almost three out of ten say it “works badly”. Among the policies belonging to the Basque Government, only the area of housing generates more concern.
We asked Félix Zubia, head of the ICUs of Donostia Hospital: “There are
doctors who work in public health while working in private. But those who leave the public and go exclusively to the private are, for the time being, very few.” It is known that this occurs, and that it is not that the story of the stories has an appointment with the dermatologist in the long term, who goes to the private clinic and is attended by the same doctor of Osakidetza. The Bridge says that those who go from one to the other to work "quantitatively not many", and that therefore it is not a serious problem for the system, but it says that it does not think it legitimate to have double activity. Moreover, those who have great responsibilities do: “Whoever has the responsibility to comply properly and should be far from private interests”.
Mikel Delgado, a fake name, knows Osakidetza internally, is an anesthesiologist and has been working for a couple of decades. The Puente knows first-hand the examples mentioned and adds that doctors who come to work privately in the afternoon give fewer appointments in the morning to get off a little earlier.
But the issue goes beyond doctors’ walking. Doctors missing? Both say yes. The Bridge considers that they are affected by short-term strategies and, above all, has focused on recruitment policies: “In 2006, many doctors who have trained have not stabilized and have been working in very poor working conditions.”
Felix Zubia: “I think you can’t work in public
and private health”
Power and interest Delgado affirms that the calls for public job offers have become “more acute” once the irregularities of 2018 have
been published. “Hiring a letter has been cut, the service chiefs had a great influence on it, as they trained the youth and they ran the tests.” And he believes that the conflicts of OSI Donostialdea are linked to this, because it has been seen that “the heads of service are at risk of their power”.
There are great power relations within Osakidetza, as Delgado believes. The senior officials and managers usually decide the Department of Health and the Government, but the anesthesiologist has emphasized that among the service heads there is a power struggle; in short, it is the doctors, but the voters: "As society itself is divided into social classes, in Osakidetza there is also a much greater separation". According to Delgado, "own elitism" directly influences this, and the holders of relatives or friends in the bottle occupy a certain position.
Mikel Delgado: "Society is divided into social classes, in
Osakidetza there is still
more differentiation"
Continuous training is encouraged to promote the development of health services and "hyper-specialisation". The heads of service of the Donostia Hospital have among their demands "to reward knowledge of specific knowledge". It is necessary to develop knowledge, but among the most critical it has a second reading: on the one hand, those of a certain economic level are the ones that can lengthen the studies, and on the other hand, specialization leads to innovation. And innovation, especially in machinery and research, starting with drugs. Behind it is a huge industry.

The privatization of health in Araba, Bizkaia and
Gipuzkoa has increased the number of people with private health insurance by 6.4 per cent over two years, exceeding 500,000 inhabitants, almost one in four territories. It's
a growing percentage. For Zubiea it is "worrying", "foreseeable", according to Delgado, "is the revelation of the polio of public services". According to the bridge, the "short-term plans" mentioned above have caused public health to "go down", and it is understandable that one has lost the benefit of the other. However, he does not believe that there has been a "plan" of his own.
Just look at Osakidetza's Strategic Plans to see "the direction of the system" according to Delgado. The issue stems from the creation of Integrated Health Organizations (OSI): "It seems like a company plan, patients become users and are not active subjects, they are defined as external agents". This is the key for Delgado to actively position citizenship. hospitals in
downtown
In the CAPV, over a period of two years, the number of private insured persons has increased by 6.4%, with a quarter of the population in the private sphere.
In 2011, OSIs were created as conciliation institutions for Primary Care and specialized care. But because the big one tends to eat small, and even more so when the private hand is involved, here too has been: in 2017 the Breathe Primary Care platform began to mobilize because workers were not heard. The first door that people cross is their own and they lack resources. In Primary Care, the worsening of many diseases can be avoided and, at the same time, consultations with specialists can be saved. However, expenditure is a significant benefit for the rear industry.
Many have pointed to "hospital centrism," and in response to criticism, Zubia says that to a large extent they are right: "You cannot put so much money into state-of-the-art technology and so little into Primary Care, you have to seek balance, give importance to one another, but while still investing in innovation."
Osakidetza has structural problems, but so does society itself. Aging has not yet become a "big problem that will become," but it will come. Public health platforms claim the need for a profound reform of Primary Care, setting as an example the current functioning. They act through quotas, so many citizens per doctor. But it is different that these citizens are young or old. Having more and more work in general. And work means money. A lot of money for those who have economic interests.
New law in progress
Next spring, the Public Health Act will be drafted in the Basque Parliament in Vitoria-Gasteiz, and broader consensus is expected or only government partners will support, approve and enter into force in 2023. This is one of the challenges of lehendakari Iñigo Urkullu, who made clear in the General Policy debate.
If the bill submitted by the Basque Government to the parties before the summer is not very tight, it would not entail major changes in the public health system. In general, it talks about the "value" of public health and the "application of health in all policies", but what it means in practice remains to be examined. The text suggests that, in view of the direction of the Decree, it seems that legislation on ventilation, sewage and water quality measures, among others, will be strengthened.
The pending bill has scope to improve and develop the public system, but the draft has few rebates. In practice, the bill relates exclusively to public health. However, it should be noted that a text of almost 100 articles does not mention mental health. It is mentioned once in prevention and health promotion activities.
The new law also speaks of the creation of two new bodies to promote coordination and participation between institutions and citizens. One is the Public Health Council and the other is the Interinstitutional Commission. The first provides for the direct participation of citizens through different types of social partners.
The bill can be found in the following link, from page 9.
It happens many times to me: look at the news and get nervous. The France revient, they say. Both the France of Le Pen and the Spanish xenophobia and supremacy, as well as the inflatable clowns, rise again and again. Merde revient. As we have heard, a group of workers from... [+]
Having worked on issues that no one has mentioned throughout the course, I was taken to the center of today, supposedly, a pneumonia, as I had an interlocution with Osakidetza not to know how to define them. And from the first call, oh, the exciting feeling of being in an... [+]
This notice is subscribed to by children and adolescents from the Mental Health Network of Gipuzkoa in Osakidetza, composed of clinical psychologists, psychiatrists of children and adolescents, nurses specialized in Mental Health, Social Workers and occupational therapists. The... [+]























